INTEGRATED AND ACTIONABLE HEALTHCARE INSIGHT
Analytics Partners introduces HxLogic, a powerful pre-built data warehouse and analytics solution for Healthcare organizations.
HxLogic provides organizations with better visibility into healthcare expense and cost management. It delivers robust information across the company value chain and helps identify opportunities to enhance quality of care while reducing healthcare expenses.
Through prebuilt intelligence dashboards, HxLogic provides hundreds of powerful metrics, alerts, and reports to healthcare professionals and providers. With this timely, complete information, healthcare professionals and providers across the organization can monitor performance, analyze key performance indicators, and compare them to performance benchmarks.You can spot deviations and act to correct them before they become problems.
HxLogic provides the in-depth analysis needed to allow you to Do More With More. You’ll be more informed, have more insights and be more successful.
HEALTHCARE PAYER SOLUTIONS
As a premier Business Intelligence and Data Warehouse Healthcare consulting firm, AP’s primary focus is implementing, training and consulting within the healthcare vertical. All of AP’s uncommon thinkers and consultants have previous healthcare payer experience from both the business and technology sides of the industry. Having an experienced partner can make all the difference: save time, reduce costs and implement more quickly with a team that knows your business.
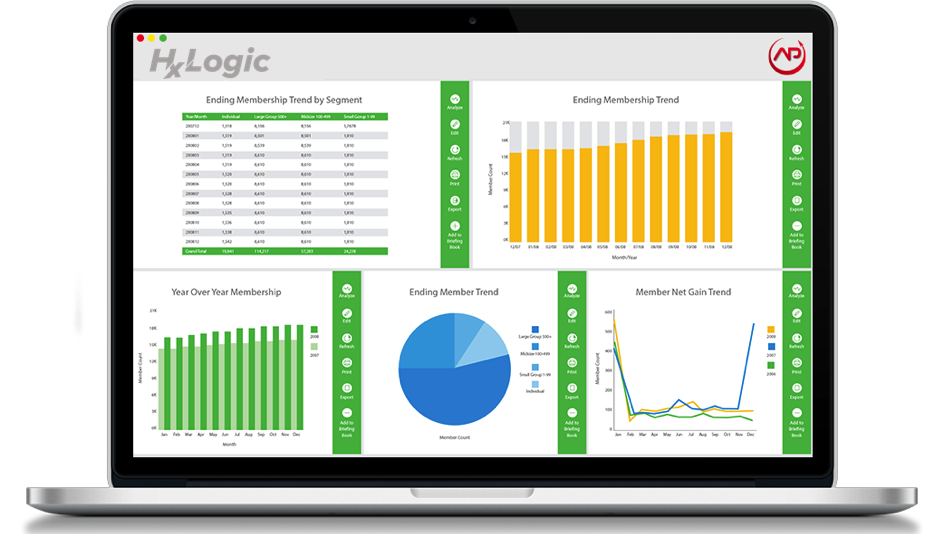
HxLogic is pre-built dashboards, reports, metrics, and alerts that provide an integrated view into Healthcare processes, quality of care, provider networks, medical informatics and cost containment.
HxLogic provides the ability to identify expense trends, DRG analysis, ER Utilization, Top Major Practice Categories along with Providers and Procedures. By enabling real time insight into an integrated information platform, this allows for advance predictive techniques to identify fraudulent claims, providers with common demographics and to improve quality of care and reduce healthcare expenses.
HxLogic provides healthcare organizations with near real time information to fundamental subjects like Claims, Members, Providers, Product, Medical informatics, General Ledger and Standardized Code Sets. HxLogic integrates all types of structured and unstructured data, including medical, pharmacy, and dental claims, as well as information about member eligibility, benefit design, providers, enrollment, public databases, demographics, websites and member experience outlets.
HxLogic comes with over 175 reports and over 750+ metrics.
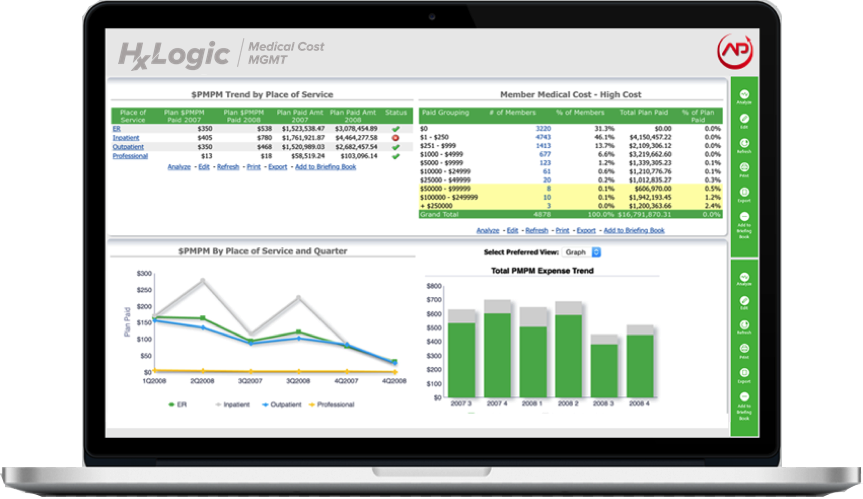
HxLogic Medical Cost Management brings actionable analytics to your organization in record time through the pre-built customizable data warehouse model, ETL work flows and Healthcare Analytics. The Medical Cost Management product comes with out of the box analytics for:

The HxLogic All Payer Claims Database (APCD) is a pre-built data model, data intake facility and analytics that saves time, money and increases the success of the project by following an industry best methodology. The HxLogic APCD is architected for multi tenants and focuses on consumer experience, benchmarking and price transparency. The HxLogic APCD product includes:
Self-Insured Solutions
HxLogic Self-Insured Analytics provides self-funded employers with the time and information to remain focused on benefits administration and vendor management. Let us focus on the tedious tasks involved with maintaining a data warehouse, landing and integrating vendor data and creating analytics. That’s what we do.

HxLogic Self-Insured Analytics automatically communicates and integrates your data from all vendor sources right into our hosted (SaaS) data warehouse model and rapidly incorporates the member data to perform analysis and assess total spend for group health benefits. Rapid and accurate data integration is imperative for Self- Insured plan administrators to be able to closely monitor their health care spend and accuracy of vendor processes and outcomes like carrier payments, disease management and wellness program effectiveness as well eligibility and pharmacy benefit management.


The value of HxLogic Self-Insured analytics is turning data into easily discernible information that allows the user to take action, make a decision or identify and prevent a problem before it impacts the bottom line.
Rapid access to actionable information is imperative for self-insured employers to be able to intervene while there is still time to influence outcomes and correct errors.


In addition to Medical Claims, Pharmacy, and Eligibility data, HxLogic Self-Insured Analytics allows group plan administrators to monitor total plan expenses by integrating additional fees and expenses associated with the administration of benefits like:
ACCOUNTABLE CARE ORGANIZATIONS
Analytics Partners (AP) is confident that your data holds the key to understanding the population for which you are now accountable. By turning your data into Actionable Analytics, we can expand your ability to analyze, measure, report and manage quality, cost and performance.
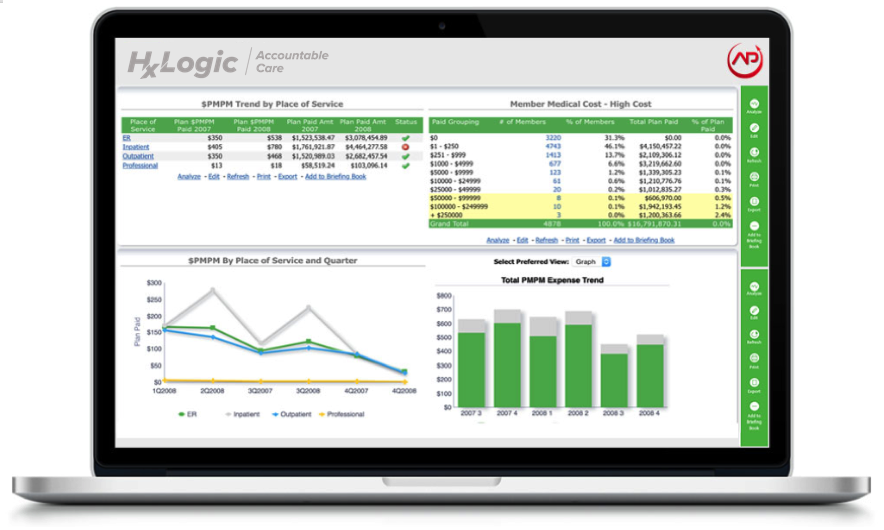
The HxLogic Accountable Care Analytics solution identifies and calculates cost savings while focusing on patient centric care.The ACO product offers an extremely cost effective and easy to use solution that automates data integration and offers prebuilt, self service and customizable analytics specifically designed to help monitor, track and improve ACO measures.
Get the full picture with complete integration of data:
Identify and Close Gaps in Care | Manage and Improve Utilization | Identify High Quality Providers
Convert data to information, information to action and action to results.
Easy Data Integration
HxLogic Accountable Care Analytics provides ACO’s with the time and information needed to remain focused on care. Let us focus on the tedious tasks involved with maintaining a data warehouse, landing and integrating CMS data and creating analytics. That’s what we do.
HxLogic Accountable Care Analytics is a 100% web-based data warehouse, data integration intake facility and analytics.
HxLogic Accountable Care Analytics automatically communicates and integrates your data from CMS right into our hosted (SaaS) data warehouse model and rapidly incorporates the beneficiary information to perform analysis. Rapid access to data is imperative for ACO’s to be able to take action on patient care while there is still time to influence outcomes.
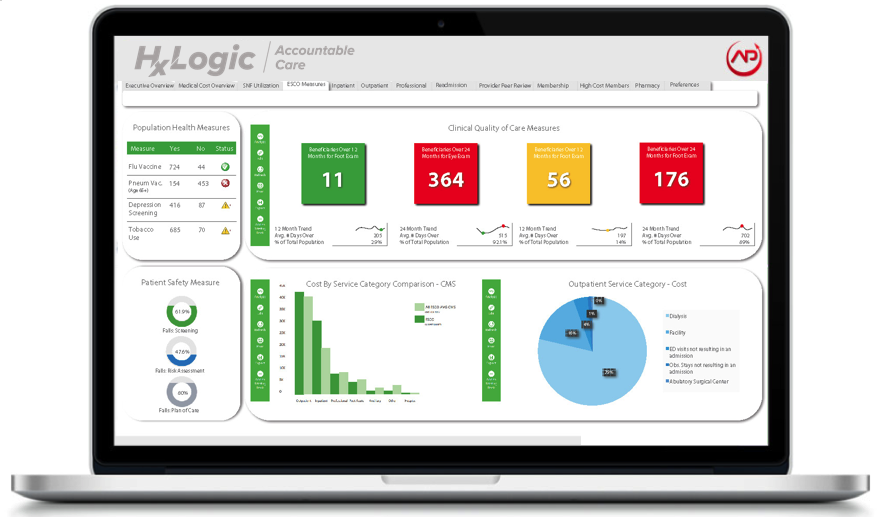
We provide the information and tools needed to influence clinical outcomes, identify and close gaps in care, monitor and track high ESRD/ESCO Measures and pinpoint causes for readmissions and the associated costs. The HxLogic ACO solution offers an out of the box ESCO dashboard that analyzes population health measures like flu vaccine, depression screening and tobacco use along with clinical quality care measures and patient safety measures
Most importantly, the HxLogic Accountable Care Analytics Solution is designed with strong data that focuses on demonstrating the results for which CMS and Payers provide incentives.
